Menu
Menu

Total Hip replacement surgery is the most common and successful joint replacement procedures in Orthopedic Surgery. Now approx. 200,000 Total Hip Replacement operations are done in USA alone every year.
Our knee joint moves millions of time to allow us to do routine activities like walking, sitting/squatting, climbing, playing, dancing etc in our life without us even knowing. Arthritis of the Hip joint makes our joint painful, stiff and deformed thereby restricting our activities significantly.
Total Hip Replacement
Total hip replacement surgery has been one of the most common and successful procedures in Orthopedic Surgery for treating patients crippled with arthritis of the hip joint.
Total Hip replacement surgery involves removing the damaged ball and socket of the arthritic hip joint. The top part of the thigh bone (femur head) is either removed and a metal implant fits within the central canal of the femur (conventional total hip replacement) or femoral head is reshapened and a metal cap fits on it (resurfacing total hip replacement). All the cartilage along with some bone is then removed from the socket (acetabulum), and a new socket is fixed in its place. This newly replaced ball and socket joint gives new joint and allow painless movement.
Total Hip replacement surgery brings dramatic relief in joint pain, correction of deformity and equalization of the limb length. Total Hip Replacement not only improves your quality of life but also gives you independence by allowing you to return to your routine activities like driving, attending offices, social functions, enjoying holidays, sports like bicycling, swimming, golf, etc.

Ceramic total hip replacement is not so new development in orthopedic surgery. These implants are designed to address some of the problems with conventional total hip replacement implants.
In the traditional (uncemented or cemented) metal and plastic hip replacement, the plastic wears out slowly over time (average 0.1 mm per year). Wearing out of plastic generates huge amount of small plastic particles (millions of particles). Over the years these plastic particles debris accumulates and trigger body response, which ultimately leads to Osteolysis and loosening of implant.
Ceramic hip replacements have been developed in an effort to decrease the wearing out of hip implants. The wear rate of ceramic hip implants is much less in comparison to conventional total hip implants, therefore, it is anticipated that these improved wear characteristics will result in a longer lasting implant.
Ceramic hip replacement is a good option in young and high demand patients with hip arthritis, as they are at high risk for early wearing out of the hip implant.
There are few issues with ceramic hip implants. As the ceramic hip implant material is hard and brittle, it can crack leading to either fracture of the ceramic head or liner (much like a ceramic dish dropped on a tile floor), although such incidences are very rare now. The other issue is squeaking noise from the ceramic on ceramic implant, which can be very annoying. However, both these issues are much less with current generation of delta ceramic.

Total hip replacement surgery is a highly successful procedure for patients crippled with arthritis of the hip joint. This operation is now done in patients at younger and younger age group because arthritis, from various causes, can damage hip joint at any age. Younger patients live longer and continue to pursue full and active life style even after hip replacement surgery. Their desire is for early and complete return of function with no limitations on their activities. Their active life style places a lot of stress on the artificial implant and affect the survivorship outcome of conventional total hip replacement surgery in younger patients inferior to those in elderly age group.
Surface Hip Replacement is different from conventional total hip replacement:
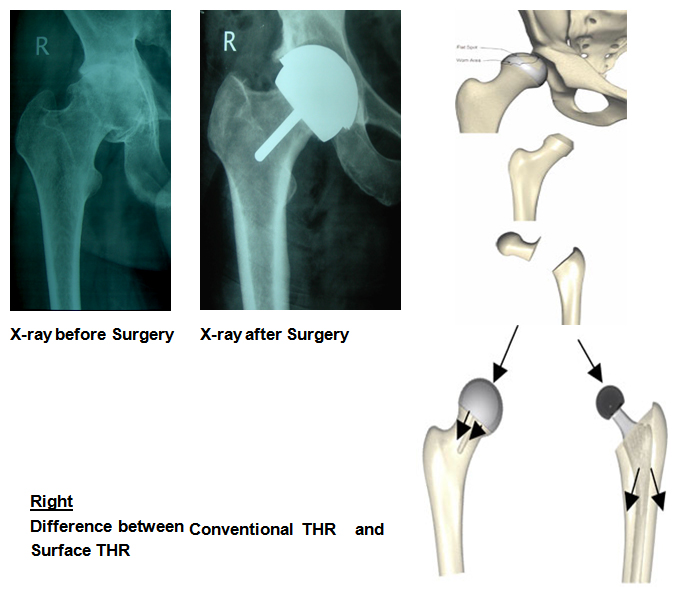
As compare to conventional hip replacement surface replacement is more stable, allows more movements, have negligible risk of dislocations and majority of them have high level of patient satisfaction. A patient can squat / sit cross-legged on floor and thereby able to pursue lifestyle activities to suite our Indian culture, something forbidden with conventional total hip replacement. Patient can also start moderate impact sports activity as well. As capping of femoral head is done and medullary canal is not violated, repeat (revision) surgery is just like doing conventional hip replacement surgery on femoral side, therefore it is also known as bone preserving hip operation. They are in use for the last 10 – 15 yrs and in these times more percentage of surface hip replacement patients are surviving in comparison to conventional total hip replacement, except for increase complication in the first few months.
Surface hip replacement is technically a high demand surgery and is not meant for every arthritic hip. We choose our patient carefully to achieve desirable success after surface hip replacement.
Concern of high metal ions in the body: As surface hip replacement has metal lining on both sides (compare to metal on plastic in conventional hip replacement) there is increase in metal ion particles concentration after surgery in patients’ blood sample, especially in the first two years. Can metal ions cause cancer in long term has been a concern, however not even a single reported case even with older generation of metal on metal prosthesis done over 30 years ago.
Similarly metal ions can cross-placental barrier; therefore women of childbearing age should be careful in choosing this option.
Patients with renal failure or those who are prone to develop end stage renal disease should refrain from choosing surface hip replacement or metal on metal prosthesis.
One has to be very selective in choosing patients for Surface Hip Replacement. These includes:
Surface hip replacement should only be undertaken after due consideration regarding metal ion sensitivity & its future implications.
Surface total hip gives you a very stable hip with virtually a normal range of motion and allows higher activity after surgery compare to conventional total hip replacement. As chances of dislocation are less, you are allowed to do most of the activities of daily living very early. However, sitting cross leg on floor and squatting is allowed after 4 – 6 months of surgery, so as to allow the artificial cup to get integrated with the bone in patient’s acetabulum or socket.
You are requested to refrain from high impact sports / jumping etc., even you see advertisement or patient story on Internet, as this increases the risk of fracture of neck of femur.
All joint replacement surgeries have some complications, however they are very few. The advantage of Surface Total Hip is that it allows the option of a total hip if it fails then a standard total hip stem can be used during revision surgery. For younger or more active patients who are more likely to cause an implant to come loose, this can be a great advantage.
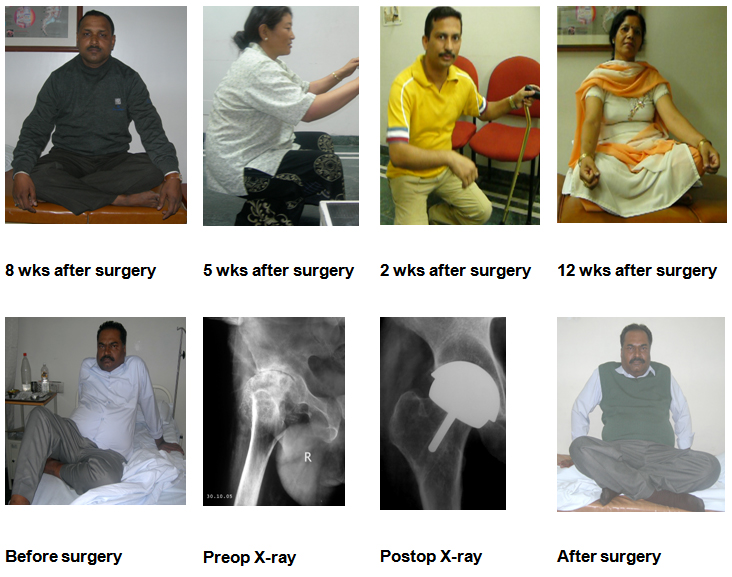

As with any major surgery, there are potential risks involved after Total Hip Replacement surgery. Even though the incidence of complications after Total Hip Replacement are small, however, their significance is high for both Patient as well as surgeon, considering the complexity of the procedure. The decision to proceed with any surgery is made because the advantages of surgery outweigh the potential disadvantages.It is important that you are informed of these risks before the surgery takes place.
Complications can be medical (general) or local complications specific to the Hip.
Medical Complicationsinclude those of the anesthesia as well as your other illness related,almost any medical condition can occur so this list is not complete. Few of them include:
Infection
Infection can occur after any operation. Being a foreign body artificial joints are always at more risk of infections especially with any dental work or other surgical procedures where germs (Bacteria) can get into the blood stream and find their way to your implant. Although infection rates after joint replacement surgery arevery low (approximately 1%), yet, even this percentage is very significant.
Lot of precautions are taken before & during surgery to prevent this complications, which includes preoperative part preparation, blood test & urine test, Antibiotics, Sterile operation rooms with laminar airflow etc. Patients with Diabetes, Rheumatoid arthritis, Psoriasis, Renal & Hepatic Compromised patients, HIV patients, h/o past infection like TB, Chronic urinary tract infection, etc. are at a higher risk for developing postoperative infections.
Early infections, low virulence infections can be treated with antibiotics, but if they do not respond to antibiotics, then further surgerylike surgical debridement (joint cleaning) may be required. If infection persist or gets aggravated in spite of adequate antibiotics / joint cleaning then your artificial joint may need to be removed and replaced by cement antibiotic spacer to eradicate infection.
If you have any unexplained pain, swelling, or redness in the operated knee joint, you should consult your surgeon as soon as possible.
Blood Clots (Deep Venous Thrombosis)
Bloodclots in the veins of the legsare one of the most dangerous complications of hip replacement surgery.They can form in the calf veinsafter surgery and can break and then travel to the lung causing Pulmonary embolism. Pulmonary embolism is serious and even life threateningcomplication. It is treated with medicines to dissolve it. Adequate precautions are taken before & after surgery to prevent them from occurring; like LMWH (medicines), Aspirin, Calf pumps, early exercises, Stockinet’s etc.Blood clots can occur despite all these precautions and are usually not dangerous if appropriately treated.If you get calf pain and sudden shortness of breath at any stage, you should notify your surgeon immediately and rush to hospital.
Leg length Inequality
The length of the leg may be changed by the surgery and sometimes very difficult to achieve right length during Total Hip Replacement Surgery. Sometimes the leg will be deliberately lengthened in order to stabilize the hip or to improve muscle function. Sometimes leg length are equal, however pelvis is tilted because of long standing deformity, and in the first few weeks after surgery, most patients complain that the operated leg feels “too long”. This is an artificial sensation, which will resolve itself over a few months.Shoe lifts may be necessary if the difference is more than a quarter of an inch. When the leg is more than four cm short to begin with, it may be impossible to equalize the legs for fear of damaging the nervesto the legs (Sciatic Nerve). Revision surgery may be required if leg length inequality bothers you persistently.
Dislocation
Dislocation means that the metal ball slips out of the plastic socket. Though not an uncommon problem after hip replacement, however the actual incidence stays low and every surgeon faces this problem. Large number of factors is responsible for this complication. Dislocations are more likely to happen in very elderly patients, alcoholics, people with weak muscles around hip. Most important thing is to prevent dislocation after surgery. It is much less with the current use of large diameter of femoral head during total hip replacement. Please carefully follow the instructions given to you during your stay. The physiotherapist will also teach you what positions to avoid, and how to safely use your hip replacement during this early phase of your recovery.
If the hip does dislocate, reduction is doneunder anesthesia. The incidence of dislocation is higher in Revision hip replacement surgery.
Aseptic Loosening
It is the most common long-term complication of total hip replacement surgery. Loosening of the prosthesis (wear & tear) from the bone is the most important long-term problem. Current generations of implant have good survivorship. Good surgery, choice of correct implant with proven design and good survivorship, regular exercises to maintain good quality of bone & muscle, maintaining weight and avoiding high impact activities are some of the factors which delay this complication. Revision Total Hip Replacement surgery is the ultimate solution.
Plastic Wear
It is another common long-term complication of total hip replacement surgery. The plastic lineris the weakest link in the implant and will eventually wears out over time. Wear of the Plastic Polyethylene Socket starts from the day of surgery. Current generations “Cross-linked” polyethylene promises a wear rate about half that of previously used non cross-linked polyethylene. Plastic wear against a Ceramic femur head and Oxinium femur head is much less in the lab. Ultimately surgery will be required to change the worn polyethylene cup if there is no Aseptic Loosening of the implant.
Damage to Nerves and Blood Vessels
It is an exceedingly rare complication. Nerve injury is more common than blood vessel injury. Total damage to the nerve happens rarely, rather mostly,the nerve get stretched especially the Sciatic nerve during the total hip replacement surgery. Damage to sciatic nerve leads to Foot Drop, which leads to difficulty in walking & an ugly gait. For severe damage exploration and repair is required. For the rest observation along with modified rehabilitation protocol is followed. Nerve may take six to nine months to recover; sometimes the damage may never recover.
Extra Bone Formation (Heterotopic / Ectopic Bone)
It is one of the less common complications and one of the commonest causes of hip stiffness after total hip replacement surgery. Small amounts of ectopic bone appear frequently around hip replacements but do not cause any problem and extensive bone formation causing severe stiffness is rare. Patients undergoing total hip replacement following acetabular fractures are at high risk and indomethacin is given post surgery to prevent it.Radiation treatment is also an alternative.It can also be treated by surgical removal of the bone, but only when it is “mature and extensive.
Fractures or Breaks in the Bone
Incidence of fractures is low, butcan occur during surgery and they can either be a crack, perforation or major fracture. Severely osteoporotic bones are at a higher risk. Minor cracks can be managed by changes in postoperative rehabilitation protocol, while major fractures are managed well with wires, cables or appropriate long implants. Sometimes fractures are noticed only on post operative x-rays, and they are managed by modifying postoperative protocol or rarely may requires resurgery.
Fracture around the implant (peri-prosthetic fractures) can happen many weeks or months after the surgery. These peri-prosthetic fractures usually require surgery.
ALVAL or “allergy to metal ions”
It is an uncommon complication seen after metal on metal total hip replacement surgery.People who know they have metal allergies should be tested for metal allergy, however, the tests are not very reliable, and so they are only performed if a metal allergy is suspected. Allergy to the plastic parts has never been reported. Some patients with metal implants have had temporary, mild skin rashes, while some have had severe rashes that resolved only with removal of the implant. ALVALis a Delayed Type of metal Hypersensitivity (DTH) is induced due to high concentrations of Cobalt and Chromium ions that build up around the joint. This leads to painful inflammation in the joint (“Lymphocytic Vasculitis”) and isalso termed as “pseudo-tumors”. Note that the term “pseudo-tumor” does not mean it is any type of cancer. Indeed, so far, after more than twenty-five years of metal-on-metal experience in Europe, there is no evidence that metal ions from a hip replacement might cause cancer.
Summary
I understand surgery is not a pleasant prospect for anyone, but for some people who are crippled with arthritis, it could mean the difference between leading a near normal life and putting whole life up with a debilitating condition.
Surgery is only offered once non-operative treatment has failed. It is an important decision to make and ultimately it is an informed decision between you, your surgeon, and your family. Surgery offers correctionof deformity, relief in pain, and restoration ofmovements to bring independence in all the activities important for daily living. With recent advances in medicines and anesthesia this is done with the least amount of possible risk.
Although most people are extremely happy with their total hip implant, complications can occur and you must be aware of these prior to making a decision. You should discuss all of your concerns thoroughly with your Surgeon prior to surgery so that you can be sure that this is the procedure for you.

Ambulation / Walking / Weight Bearing
Usually allowed on next or 2nd postop day with both cemented and uncemented total hip implants. However, there may exception to this, especially in revision total hip replacement or few difficult primary total hip replacement cases like acetabular fractures. For ambulation initially a walker is used to start with, followed by progression on to a cane / stick. You are allowed to put as much weight as you can on your operated leg (with the help of the walking aid in most cases). If using a cane, use it on the other side as your hip replacement. This not only helps you in unloading your operated hip, but also prevents you from falling over while your muscles around the hip recover.
In case of Uncemented Total Hip Replacement Implant it is advisable to use cane for 3 month after the surgery. This helps in better bonding between the implant & the bone, essential for the longevity of the implant.
Dressing and Incision care
Bathing is usually not allowed until the stitches come out in 2 weeks. If the dressing appears soaked from underneath then please inform us immediately. The dressing applied in the hospital on the day of discharge can be left on until removed by us at 2 weeks (day of suture removal).
Pain Medicine
Pain medication often is needed for 3 to 6 weeks after total hip replacement. If however one feel severe pain or spasm, use ice packs besides calling your doctor or taking SOS additional pain medicine. Please remember that if you are taking pain medicine, you MUST avoid alcohol and banned drugs.
Diet
You need to eat to gain back your strength. You should resume your pre-hospitalization diet unless otherwise instructed.
Exercise and Activity at home
Recovery after total hip replacement is less painful and earlier than total knee replacement. Hip exercises will help you regain your mobility faster & better. The exercises should not cause severe pain. If they do, either inform your physical therapist, surgeon or stop those exercise from your schedule for a while. Exercises should be done 3 – 4 times a day.
Climbing Stairs
The following instructions are useful for climbing and descending stairs.
In case of unilateral (one hip) total hip replacement:
| UPSTAIRS | DOWNSTAIRS |
| The non-operated leg goes first. The operated leg goes second. The crutches go last (at the same time as the operated leg) |
The crutches go first The operated leg goes second The non-operated leg goes last |
“If you have bilateral hip done then stronger leg goes first”.
When can I drive?
You should not drive as long as you are taking narcotic pain medications. It largely depends on your progress of recovery, however 3 to 6 weeks is a good time to drive for most if not for all.
When can I return to work?
Return to work is earlier after total hip replacement as compare to total knee replacement. It’s never a mistake to take more time off in the beginning of the recovery as you can focus on your hip better. Depending on your occupation it takes 3 to 6 weeks after surgery to start office or light activities. Keep in mind that you need to be using crutches / cane.
My hip clicks after surgery
Usually clicking after surgery is not abnormal. The clicking is a result of soft tissue moving across the front of the hip or the metal parts coming into contact with one another. This sensation usually diminishes, as your muscles get stronger. “If it persist, increases or gives you a sense of instability, then please contact your surgeon”.
How To Prevent or Reduce Leg & Ankle Swelling
Fluid can accumulate in the legs due to the effects of gravity. Usually it is not a problem in the hospital, but it gets worse when you go home or rehab because you are doing more.
Do’s and Don’ts after Your Total Hip Replacement
Below is a general list of precautions to follow after your total hip replacement.
Lying Down
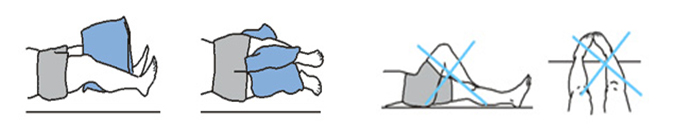
Sitting
Usually chair sitting is started in the hospital. Use a high chair for initial 6 to 12 weeks preferably with a side handle.
| Do: | Don’t (Avoid): |
|
|
| Other positions to avoid following Total Hip Replacement | |
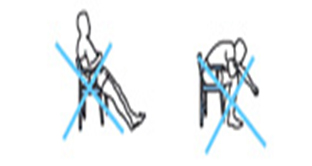 |
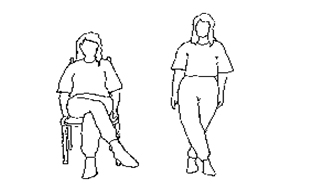 |
You must call your doctor!
If you experience any of the following problems

What is a revision Hip Replacement?
Revision hip replacement surgery is a procedure in which an existing prosthesis is revised or replaced with a new total hip implant. An original total hip implant has two broad components, one on femoral side and other on acetabular side. Each of these components also has further subcomponents, for example an uncemented cup has an outer shell and inner polyethylene (plastic) liner, while femoral component has stem and modular head.
Thus a revision total hip replacement can be a revision of all the components or revision of one component, for example only change of polyethylene (plastic) liner.
Revision total hip replacement surgery is a demanding surgery, but the results are good in the vast majority of patients, though not as good as primary total hip replacement surgery.

When is it needed?
The Primary total hip replacement is a very successful operation with high survival rate for 10-15 yrs. The problem, unfortunately, is that slowly and progressively, hip replacements wear out over a period of time. 15 years after a hip replacement, there is a 90 – 95% chance that the implant will be functioning well. 20 years after surgery, the chance is about 80% and it keeps reducing progressively over the years. A loose hip implant tends to be painful and unstable, therefore patients who wear out their prosthesis will require a revision hip replacement surgery
Hip replacements can wear out for a variety of reasons. By far the most common cause of wear is Aseptic Loosening.
Other causes for revision hip surgery are Infection, repeated Dislocations, Osteolysis (development of loose bone cavities around hip implant without loosening of implant), Periprosthetic Fractures (breaking of the bone around the prosthesis), Implant Fracture (breaking of the prosthesis) etc.
Depending on the cause of the implant failure, sometime treatment other than direct revision hip replacement may be necessary. For example, in the case of infection, the hip implant may need to be removed to treat the infection, an antibiotic spacer need to be inserted along with few weeks of antibiotics, and once infection is controlled then revision hip replacement is performed.
How different is revision hip surgery different than primary total hip replacement?
The principles of revision THA are similar to those of primary hip replacement surgery. However, revision hip surgery is more challenging and complicated than primary hip replacement. Poor quality of the patients bone often makes it difficult to achieve stable fixation of revision hip implants. Furthermore, removing the previous knee implants not only necessitates more extensive surgery, but also adds to loss of bone to the already limited patient bone stock (remaining bone).
Also not only do the patients tend to be older, but also the surgery time is longer and the blood loss is greater during or after surgery adding to the difficulty of revision surgery. Together, these problems make revision hip replacement much more complex surgery.
Revision hip surgery on an infected hip requires two or more separate operations. In the first operation, the old hip prosthesis is taken out and a block of cement mixed with high dose of antibiotics (antibiotic spacer block) is inserted in the joint for 6 – 12 weeks. This block acts as a spacer and also releases high concentration of antibiotics in the hip joint locally. The patient is also given intravenous antibiotics for 6 weeks, and constantly evaluated with repeated TLC, DLC, CRP and ESR. After the infection has cleared, the hip is reopened and the new revision prosthesis can be implanted.
During the revision surgery one may need special implant like longer and wider stems, cages, rings, bone graft, mesh, etc. Though these implants are expensive and have some limitations, but indispensable (in certain situation) to achieve good stability of revision implant.

How revision total hip replacement can help me?
The revision total hip replacement surgery is a successful and durable operation, though not as much as primary total hip replacement surgery. You can expect significant improvement in your symptoms after revision hip surgery, which includes:

How do I know when I need revision hip replacement?
If your pain is increasing, if you are having difficulty in walking or you have to use a support for walking, if you are having instability on getting up, if you having repeated hip joint dislocations, or there is continuous discharge from the operative scar not responding to any treatment, then its time for you to consult your doctor for the possibility of revision total hip replacement.
Sometimes you may have few or no symptoms, but the x-rays show a big osteolysis next to the implant necessitating a revision hip replacement. Some other time you may be very symptomatic, and x-rays also show gross malalignment or loosening of components or change in the position of components or you has sustained periprosthetic fracture, you will be better off with revision hip surgery.
The decision and extent of revision hip replacement depends on cause of revision hip surgery, severity of discomfort, x-rays, blood investigations like CRP, TLC, DLC or ESR and your overall clinical condition. At times you will be requiring to undergo special investigations like Tc99 Bone scan / I111 bone scan or MRI scan to confirm the diagnosis and assess true extent of lesion. It is essential to remove a loose or damaged prosthesis before irreversible harm is done to the joint and surrounding bone.
Underlining the complex nature of surgery, the right time for revision hip replacement can be decided by you together with your Orthopedic surgeon in consultation with Physician and Anesthetist.
If you have a hip replacement and think you may need revision surgery, you must discuss your options with your orthopedic surgeon.
What should I expect during my hospital stay?
Before Surgery: Most of the patients are admitted two days before surgery and undergo a through medical checkup which includes evaluation by the treating surgeon, anesthetist, intensivist, and physiotherapist besides investigations like Chest X-rays, ECG, blood (including CRP, ESR, TLC & DLC) and urine test. X-ray images of pelvis with hip and thighbone from different angles are taken to plan your surgery. You may require whole body bone scan or CT / MRI of the hip joint to assess the bone loss around implant. At least 2 – 3 units of blood may be necessary. Careful control of blood sugar is done in Diabetic patient before surgery.
Hip joint is scrubbed with soap and water, painted with betadine solution, and then covered with a sterile drape in your room a night before your operation.
Surgery: Preferable choice of anesthesia is Spinal anesthesia (it anesthetize both legs only) with sedation. The duration of surgery ranges from 2 to 3 hrs. You will be kept in a recovery room for one day for the monitoring of vital parameters. You will be requiring abduction pillow (a pillow between the legs to keep them wide apart). Knee / static quadriceps and hip abductor exercises are started on the day of surgery.
After Surgery: On the 3rd day your drainage tubes will be removed while on 4th day your dressing will be changed. In most cases a knee immobilizer will be worn. Knee bending on the CPM machine is started 2-3 days after surgery; bedside sitting is started on the 4th day while walking with support and toilet training are started from 5th day onwards.
Most patients can ambulate comfortably with the support of a stick or walker, bend knee up to 800 to 900, start going to toilet and are also able to climb a flight of stairs. Most patients are comfortably discharged on 7th to 8th day.
What happens after I go home?
Aftercare following hip revision surgery is essentially the same as for primary hip replacement, consisting of a combination of physical therapy, rehabilitation exercises, pain medication when necessary, and a period of home health care or assistance.
You will be requiring antibiotics for a longer time as compare to primary total hip replacement surgery especially if you are a diabetic, rheumatoid arthritis patient or infection was the cause of revision hip surgery.
The recovery time after revision hip replacement surgery depends on the cause of revision and may vary from 4 to 8 weeks.
What are the risk following Revision Total Hip Replacement?
The complications following revision hip surgery are similar to those for primary hip replacement surgery and include:

As we know that slowly and progressively, hip replacements components will wear out over a period of time. In all likely hoods you have good chance of revision after 15 to 20 years of your primary hip replacement surgery.
With wear and tear plastic cup thins out, there is loss of bone around the stem and cup and gradually the implants become loose. A loose hip implant tends to be painful and unstable, therefore patients who wear out their prosthesis will require a revision hip replacement surgery
Sometimes a revision total hip replacement can be a revision of all the components or else revision of one of the component, for example only change of polyethylene (plastic) liner.
Revision total hip replacement surgery is a demanding surgery, but the results are good in the vast majority of patients, though not as good as primary total hip replacement surgery.
If your pain is increasing, if you are having difficulty in walking or you have to use a support for walking, if you are having instability on getting up, if you having repeated hip joint dislocations, or there is continuous discharge from the operative scar not responding to any treatment, then its time for you to consult your doctor for the possibility of revision total hip replacement.
When is it needed?
The Primary total hip replacement is a very successful operation with high survival rate for 10-15 yrs. The problem, unfortunately, is that slowly and progressively, hip replacement wears out over a period of time. 15 years after a hip replacement, there is a 90 – 95% chance that the implant will be functioning well. 20 years after surgery, the chance is about 80% and it keeps reducing progressively over the years. A loose hip implant tends to be painful and unstable, therefore patients who wear out their prosthesis will require a revision hip replacement surgery
Hip replacements can wear out for a variety of reasons. By far the most common cause of wear is Aseptic Loosening.
Other causes for revision hip surgery are Infection, repeated Dislocations, Osteolysis (development of loose bone cavities around hip implant without loosening of implant), Periprosthetic Fractures (breaking of the bone around the prosthesis), Implant Fracture (breaking of the prosthesis) etc.
Depending on the cause of the implant failure, sometime treatment other than direct revision hip replacement may be necessary. For example, in the case of infection, the hip implant may need to be removed to treat the infection, an antibiotic spacer need to be inserted along with few weeks of antibiotics, and once infection is controlled then revision hip replacement is performed.
How different is revision hip surgery different than primary total hip replacement?
The principles of revision THA are similar to those of primary hip replacement surgery. However,revision hip surgeryis more challenging and complicated than primary hip replacement. Poor quality of the patients bone often makes it difficult to achieve stable fixation of revision hipimplants. Furthermore, removing the previous knee implants not only necessitates more extensive surgery, but also adds to loss of bone to the already limited patient bone stock (remaining bone).
Also not onlydo the patients tend to be older,but also the surgery time is longer and the blood loss is greater during or after surgery adding to the difficulty of revision surgery. Together, these problems make revision hip replacement much more complex surgery.
Revision hip surgery on an infected hip requires two or more separate operations. In the first operation, the old hipprosthesis is taken out and a block of cement mixed with high dose of antibiotics (antibiotic spacer block) is inserted in the jointfor 6 – 12 weeks. This block acts as a spacer and also releases high concentration of antibiotics in the hip joint locally. The patient is also given intravenous antibiotics for 6 weeks, and constantly evaluated with repeated TLC, DLC, CRP and ESR. After the infection has cleared, the hip is reopened and the new revision prosthesis canbe implanted.
During the revision surgery one may need special implant like longer and wider stems, cages, rings, bone graft, mesh, etc. Though these implants are expensive and have some limitations, but indispensable (in certain situation) to achieve good stability of revision implant.

X-ray of a 83 yrs old gentleman presenting with hip pain and difficulty in walking after 16 yrs, showing Asceptic Loosening 3 yrs Post Revision THR
How do I know when I need revision hip replacement?
If your pain is increasing, if you are having difficulty in walking or you have to use a support for walking, if you are having instability on getting up, if you having repeated hip joint dislocations, or there is continuous discharge from the operative scar not responding to any treatment, then its time for you to consult your doctor for the possibility of revision total hip replacement.

What is OXINIUM material and how is it made?
OXINIUM (Oxidized Zirconium) is a new material used for manufacturing components of total hip implant. First, the zirconium alloy metal is shaped into an implant component and thereafter; the implant is put through a patented process, which allows oxygen to absorb into the zirconium metal. Once the surface of the metal is saturated with oxygen, it changes from metal to ceramic.
This ceramic surface gives the OXINIUM material significant advantages over cobalt chrome. And because only the surface is changed, the rest of the component is still metal and retains its overall strength.
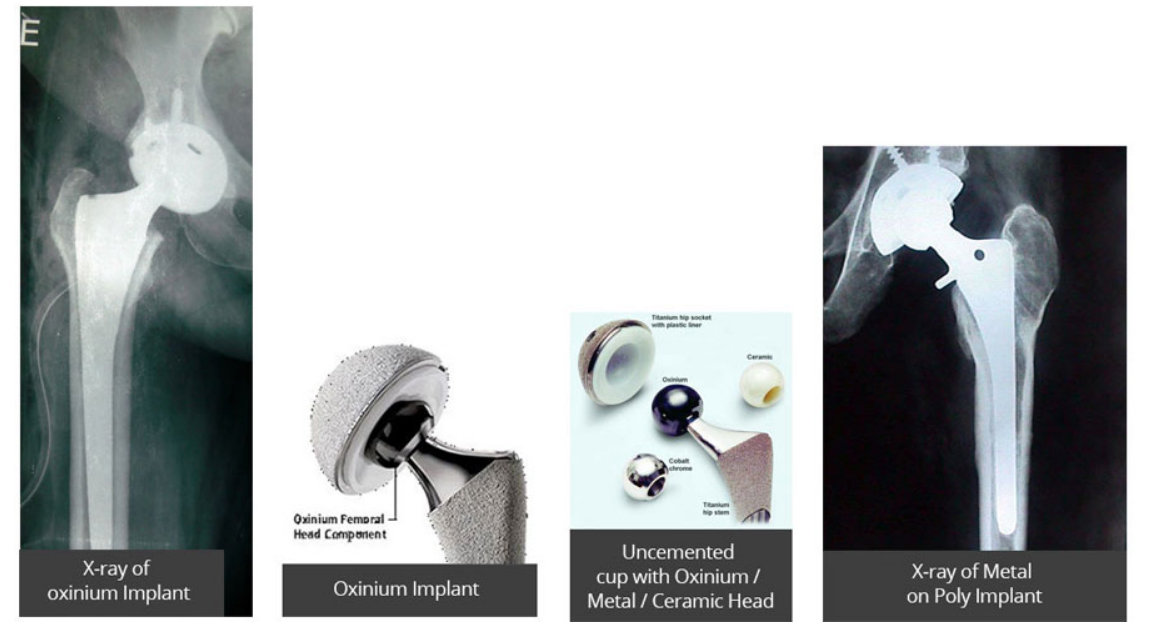
What are the advantages of OXINIUM?
It actually incorporates the best features of all available material options (both ceramic and cobalt chrome) with fewer material related risks due to its superior hardness, smoothness and resistance to scratching and abrasion. All of which makes for a potentially longer-lasting, superior performance as it is vastly superior to commonly used cobalt chrome surfaces.
Now a younger patient with advanced arthritis no longer has to suffer for years until he or she reaches an appropriate age for joint replacement surgery. An Oxinium hip is a very good choice for young patients suffering with advance arthritis, and is available in various head sizes 28mm, 32mm and 36mm.
In fact patients who want to return to an active lifestyle, which include low impact activities like dancing, gardening and stationary cycling, may also benefit from Oxinium hip replacements due to the fact that they are better able to tolerate these activities and still may last longer than traditional joint replacements.
How do scratching and friction affect a hip implant?
Traditionally, cobalt chrome has been the material of choice for hip implants because of its strength and relative hardness. However, studies have shown that, after implantation in human body, cobalt chrome implants have a tendency to roughen over a period of time. Thus, when a roughened implanted joint surface rubs against a plastic bearing surface, the plastic wears out. After repeated rubbing over time, the plastic surface simply wears out and additional surgery is then needed to replace the worn implants. Laboratory studies have proven that a scratched or roughened cobalt chrome implant will dramatically increase production of plastic wear debris and reduce the life span of the hip implant.
How long will an OXINIUM total hip last?
According to laboratory wear testing, OXINIUM implants demonstrate the scratch and wear resistance necessary to be potentially longer lasting as compared to traditional artificial hip joints. The smooth, hard surface of an OXINIUM implant is not a coating, but the result of a process, which allows oxygen to absorb into zirconium metal, which changes only the surface from metal to ceramic. The ceramic surface makes OXINIUM implants 4,900 times more abrasion resistant than cobalt chrome. It also reduces friction between the implant and the plastic surface for superior durability over time.
Are people who are nickel sensitive candidates for OXINIUM hip implants?
There is no detectable nickel in the OXINIUM material, the leading cause of negative reactions in patients with metal allergies. The OXINIUM material is one of the most biocompatible metals known to man and most immune systems are able to tolerate the new implant. Furthermore, OXINIUM is the only orthopedic metal that does not contain nickel. Patients who have needed hip replacement surgery but could not tolerate the nickel content of traditional implants may now have the surgery they need with less fear of an allergic reaction.
If you feel that we can be of any assistance please take a moment to fill out the enquiry form below and one of our staff members will answer your question as soon as possible.
Follow us on social media and keep up to date with all the latest news from the Dr vivek mittal clinic.